Here’s how I got my cholesterol levels down
The most trustworthy source of food and
fitness journalism in the country.
Welcome to Truth Be Told, a weekly food & fitness newsletter. New here? Read our manifesto: a note on why we exist.
In August 2021, I was in the best shape of my life. My gym performance was at its peak, my abs were chiseled, personal lifting records were broken every week, and my food intake was optimal.
Physical health was sorted. Or so I thought.
I lost a cousin in his early 30s to a sudden heart attack, which shook me. He worked hard to build a career in the cutthroat world of edtech and didn’t actively exercise or monitor his diet. But there were no visible signs of something going wrong, and he’d been doing fine.
That made me wonder if my body was doing okay on the inside. Is there anything I could do to reduce the risk of a sudden stroke?
Because they’re not uncommon, just look at the news. Even athletes and celebrity actors succumbed to heart attacks. Young and otherwise fit people dying suddenly does raise questions.
Taking a closer look
So I decided to monitor and take a closer look at my heart health. My family history of diabetes made it even more crucial.
The immediate step was to get a complete cholesterol test, also called a lipid profile, which is part of the comprehensive blood test. The results of my August 2021 test were revealing. My total cholesterol levels were high, even though I was in my best physical shape — my body fat percentage was 11%, a marker of athlete-level fitness.
Meaning: My physical appearance was hiding a crucial fact about my heart health. I was unhealthy despite my well-defined abs.
I consulted a doctor and what followed was a long journey to do the ‘inside work’ and set the blood markers right. Finally, in 11 months, after several ups and downs, I did get it right. I am writing to share how I got there and the lessons I learnt.
Let’s start with the fundamentals.
Cholesterol explained
Cholesterol gets a bad rep, but it isn’t as evil as we may believe.
It’s a waxy substance, and your body needs it to build cells, produce hormones and make vitamins — it’s essential to life but in the right quantity.
The cholesterol in your blood comes from two sources: your liver and food. When we eat foods that are high in saturated and trans fats, it causes our liver to produce more cholesterol. In some people, this excess cholesterol can veer toward unhealthy levels.
Most cholesterol is found in our cells, supporting essential biological functions, and about 7 per cent floats in your blood. Of this 7 per cent, one-third is ‘good’ cholesterol, and two-thirds is ‘bad’. This is why getting a complete lipid profile is important — an imbalance in the two types of cholesterol is risky for your heart, and monitoring your stats could help prevent a sudden mishap.
What’s also crucial is to remember that there is no fixed formula that can predict why exactly someone’s heart would fail.
In his bestselling book The Body, Bill Bryson wrote:
“All forms of heart failure can be cruelly sneaky. For about a quarter of victims, the first (and, more unfortunately, last) time they know they have a heart problem is when they suffer a fatal heart attack. No less appallingly, more than half of all first heart attacks (fatal or otherwise) occur in people who are fit and healthy and have no known obvious risks. They don’t smoke or drink to excess, are not seriously overweight, and do not have chronically high blood pressure or even bad cholesterol readings, but they get a heart attack anyway. Living a virtuous life doesn’t guarantee that you will escape heart problems; it just improves your chances.”
I agree with Bryson, and I’d learnt my lesson only after losing someone.
Understand your test results
But let’s not downplay the importance of blood markers. While nothing can guarantee the absence of heart failure, keeping my total cholesterol levels under 200 mg/dl would help minimise the risk.
And that’s the key point I want to make today: get your blood tests done, understand what those numbers mean, and make incremental improvements to get those right.
That’s what I did.
Reading a blood test report can be confusing. When I started, I only knew that if a certain reading was in bold, it meant it wasn’t in the correct range. But I did not know what it meant.
I realised it’s not that complicated—just five things you need to know to understand your test results.
Like what you see so far?
Get TBT articles in your inbox every Saturday
One: How’s cholesterol measured?
Cholesterol is measured in milligrams per deciliter (mg/dL). When you check your cholesterol, the lipid profile test contains the levels of cholesterol (HDLC and LDLC) and triglycerides in your body.
Two: Good cholesterol versus bad
Our body has two types of cholesterol: low-density lipoprotein cholesterol (LDLC) and high-density lipoprotein cholesterol (HDLC).
LDL cholesterol makes up most of your total cholesterol levels. The desired level is below 120 mg/dl. HDL cholesterol should be between 40 and 60 mg/dl.
HDLC and LDLC are often referred to as ‘good’ and ‘bad’, respectively, but this simplistic classification isn’t accurate. Both types of cholesterol are the same. What’s different is the protein composition and the roles these proteins play in our bodies. HDL carries cholesterol from the body to the liver for disposal while LDL helps cells absorb cholesterol to perform important microbiological functions.
The problem with LDL — and why it’s called ‘bad’ — is that it can form a thick, hard deposit on the inside of our arteries. This narrows the arteries overtime — over the years! — making them less flexible. If a blood clot forms and blocks one of these narrowed arteries, it can result in a stroke or heart attack.
Three: Then there are triglycerides
It’s fat stored as unused calories and provides your body with energy.
If you regularly eat more calories than your body requires—especially from high-carb foods—your body starts storing a lot of unused calories, and your triglyceride levels
keep increasing. High triglycerides are a ‘silent’ killer, and there is a fourfold increase in the chances of a heart attack due to this.
Triglyceride levels above 150 mg/dl are considered high.
Fourth: Total cholesterol
It is the total amount of cholesterol in your blood based on your HDL, LDL, and triglycerides numbers. In adults, high cholesterol means having total cholesterol above 200 mg/dL.
Fifth: Ratios help predict the risk of heart disease.
Two are significant, and you’ll find them in your blood test report.
A) LDLC: HDLC Ratio: The lower the ratio, the better it is for you. The ideal range is between 3.5-1.
B) Triglyceride: HDLC ratio: This should remain below 2.
These are the basics. Onto my journey.
Initial diagnosis: August 2021
My doctor asked me to change my lifestyle after looking at my initial test results. For one, he asked me to introduce more carbs into my diet and follow a balanced approach. I’d been on a low-carb diet at this point: going low on carbs means the diet is dominated by proteins and fats, which are more satiating than carbs, which means you do not tend to binge on more calories, which helps in maintaining a low body fat percentage, which is needed for those abs.
Second, he also asked me to monitor my alcohol intake. I used to go out drinking with my friends every other weekend and binge on five to six large hard alcoholic drinks. The doc suggested that too could have led to elevated LDL levels.
First phase: August 2021 to March 2022
Things did not get better. My March report showed a further rise in LDLC levels. One reason: drinking too much. Yes, I was working on improving my cholesterol levels, but I fell for the social FOMO — so I could not resist.
Sleep was another possible factor. My bed timings were off point, which disrupted the total number of hours on many days. Some days I slept much more than needed.
Both of these lead to poor body recovery, leading to poorer quality workouts and the results show up in a less-than-optimal blood test.
Second phase: March 2022 to August 2022
Finally, my blood work improved through a lower LDLC level, lower total cholesterol, and improved HDL/LDL parameters.
Here is what worked for me:
One: Controlled Drinking
In these months, I went cold turkey for drinks on those weekends. So that’s a significant factor. I have worked on this habit now and learnt to control social FOMO.
Two: Found a middle ground for my diet
Changing my diet had a conflict.
I’d been following a low-carb, high-protein diet with a fasting period. While this improved my triglyceride/HDL ratio, it also led to an increase in my LDL. But some research said that in itself does not necessarily mean it is a bad thing; some said reducing LDL is critical.
So what to do? My target was to bring LDL below 100 while ensuring that my triglyceride/HDL ratio and HDL/LDL remained healthy.
So as per my doctor’s advice, who asked me to take the middle ground, I introduced gradual changes and started taking in more calories (within a limit, of course, just more than what I was eating earlier) to accommodate more carbs in my diet while keeping my protein intake consistent. I specifically increased my complex carb intake — whole grains, for example.
The latest report suggests that possibly worked. It’s all about trial and error.
Three: Changed my cooking oil
I paid attention to the quantity of oil being used but not the quality — but quality matters. I used to cook my food in refined rice bran or sunflower oil. Not a good idea. I switched to cooking all my foods in cold-pressed coconut oil or ghee and occasionally in cold-pressed groundnut oil. Coconut oil reportedly nudges up HDL C levels.
Remember: The benefits of a protein-rich and home-cooked meal could get negated by choosing the wrong type of oil to cook it in. Include healthy fats and proteins as a part of your meals as they help to keep cholesterol in check.
Fourth: Started taking a tablet of magnesium glycinate before sleep.
Lack of sleep is known to cause an increase in cholesterol levels. In addition, a study showed that individuals who get less than 6 hours of sleep saw a rise in their LDLC and triglyceride levels.
So I worked on improving my sleep. I have written about my experiments with sleep before. One thing I want to highlight: studies have shown that magnesium intake aids in better sleep and muscle recovery and also helps improve lipid profiles. So I started taking a tablet before going to bed.
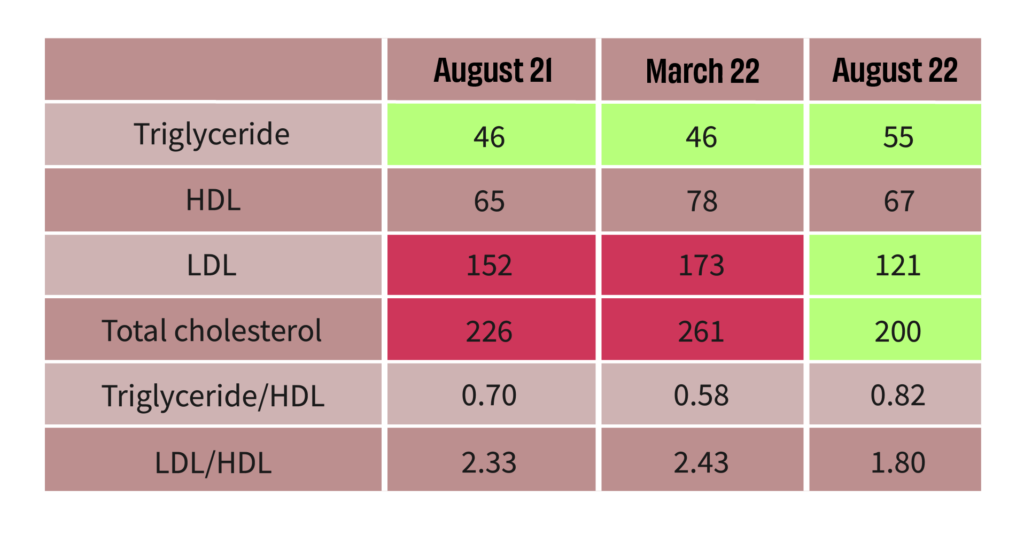
Before and after of Ankush’s cholesterol results
The table above maps the results of my lipid profile over a year. In August 2022, my body fat percentage was 16% —more than the 11% mark I had a year ago, but at the same time, I was able to bring down my total cholesterol and keep my ratios in check.
Now don’t get me wrong, it is scientifically proven that lower body fat percentage is a sign of improved metabolic health but the process of chasing that physique could lead to problems. Let’s not lose our sanity while chasing vanity. The next time I am chasing a chiselled physique, my approach will be totally different so that it does not adversely impact my lipid profile.
Heart diseases are sneaky. They don’t announce; they just arrive — I learnt this the hard way. So it’s important to keep a tab on your blood markers (even if you look healthy), consult a doctor when in doubt, and see what works to keep you healthy.
Click the logo to sign up for the newsletter
More from Truth Be Told
Safest cooking utensils for healthy living
Your brain needs to relax and here’s how you can do it
Why you can’t eat just one chip
The Definitive Guide to Smart Food Shopping
I solved the mystery of the afternoon slump with CGM
Eight swaps to eat better everyday
Diwali indulgence won’t make you fat
What spikes your blood glucose?
Is your body ageing gracefully?
Should you count calories?
Letters to Editor: Reader Response 01
My experiments with sleep
8 tips to choose the right cooking oil
You can’t be ‘healthy’, if you don’t know what it means
Food and fitness journalism is broken. We are fixing it.


